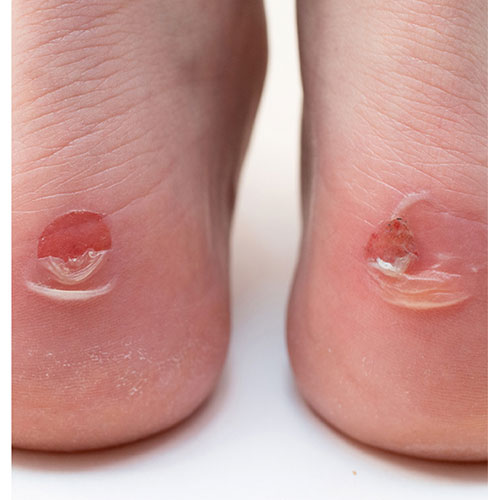
Why Diabetic Foot Ulcers Demand Extra Attention in SNFs
Diabetic foot ulcers (DFUs) are one of the most common and serious complications of diabetes. In skilled nursing facilities (SNFs), residents often have multiple health conditions, limited mobility, and reduced sensation in their feet — factors that make them especially vulnerable. If not treated quickly, these wounds can become infected, increase the risk of amputation, and lead to costly hospital transfers. Recognizing the warning signs and responding promptly can dramatically change the outcome for residents.
Early Detection Is Key to Better Outcomes
The first step to preventing complications is identifying diabetic foot ulcers early. Regular foot and skin checks performed by nursing staff allow even small wounds or pressure spots to be noticed before they progress. Interactive wound documentation and immediate communication between caregivers, attending physicians, and wound care specialists ensure no time is lost. Standardized wound assessment protocols and evidence-based guidelines help staff spot issues faster and act decisively, reducing hospitalizations.
Bringing Wound Care to the Resident’s Bedside
Once a diabetic foot ulcer is identified, fast and effective treatment is critical. Skilled nursing facilities have a unique advantage here — on-site clinical expertise and continuity of care. This makes it possible to start wound debridement, infection control, offloading techniques, and advanced dressings without delay. Facilities that use visiting wound care specialists or telehealth consultations can create individualized care plans, accelerating healing and reducing the risk of complications.
Creating a System to Prevent Hospital Transfers
Preventing hospital transfers isn’t just about clinical treatment — it’s about systems and teamwork. Adequate staff training, clear care pathways, and strong relationships with podiatrists, vascular surgeons, and primary care physicians strengthen an SNF’s wound care program. Coordinating timely lab tests, imaging, and medication adjustments also helps reduce delays in treatment. Facilities that integrate electronic medical records (EMRs) with wound care documentation see better tracking, improved compliance, and stronger communication across the care team.
The Bottom Line for SNFs
Reducing diabetic foot ulcer–related hospital transfers is a win-win for everyone. Residents experience faster healing, fewer complications, and greater satisfaction. Facilities strengthen their quality metrics, improve compliance with regulatory standards, and control costs. By emphasizing timely treatment, continuous monitoring, and interdisciplinary collaboration, SNFs can position themselves as leaders in chronic wound care.